Как сочетаются почечные заболевания с физкультурой и спортом?

Chronic Kidney Disease (CKD) is a global public health issue. Patients with CKD usually demonstrate reduced physical activity and performance.
In addition, the risk for cardiovascular events increases as the glomerular filtration rate decreases and it is estimated to be 10 to 20 times higher in patients with CKD than in the general population. Physical exercise has proven to contribute in preventing and / or improving many chronic conditions. Current international guidelines suggest that CKD patients participate in an exercise program that is compatible with their cardiovascular health, however, it is rarely recommended in a specific and clear manner to patients.
What is the definition of "exercise"?
Exercise is defined as a programmed, structured and repetitive bodily movement with the intent to improve or maintain the physical fitness level. A simple example could be 30 minutes of walking that improves aerobic exercise over time.
In what way does physical exercise positively affect CKD patients?
- It reduces the rate of decline in renal function
- It improves maximum oxygen consumption, lipid profile, mental health and sleep habits
- It reduces systolic blood pressure
- It leads to better weight control
- It increases physical performance, flexibility and performance
What are the reasons that often prevent patients with CKD from exercising?
It is evident that the most important obstacles are the fear of injury and the concern about a possible deterioration of the renal function, which leads to the conclusion that information about the specific topic is incomplete.
What type of physical exercise is suitable for CKD patients?
There are two kinds of physical exercise: isotonic (aerobic) that burns more calories such as walking, running, cycling, soccer, basketball, swimming and isometric (anaerobic) such as lifting weights, springs. The most commonly studied type of exercise intervention in CKD patients is aerobic exercise. However, isometric can also offer other benefits, such as increased muscle strength and function.
How much should a patient with CKD be trained?
It is especially important that the patient's physical activity program maximizes the benefits, and at the same time minimizes the possible risks associated with it. CKD patients should be aware of their physical limits and stop exercising when they feel tired, sick or dizzy, or difficulty in breathing. In addition, exercise therapy should be discontinued if the patient has a fever, his general condition worsens, or suffers from another disease that exacerbates exercise.
When is the best time of day for the patient with CKD to work out?
At least one hour after meals, not during the hot hours, and not within three hours before bedtime.
What are the components of an exercise program?
- The type and number of repetitions of each recommended exercise for each session
- Frequency of sessions
- The duration of each session
- The intensity of each session
Exercise programs should start at low intensity gradually increasing, depending on the patient's tolerance. This helps in reducing the risk of injury and increases the likelihood that the patient will continue to exercise. In order to achieve and maintain good physical fitness and well-being, it is best for elderly patients with CKD and other comorbidities (eg cardiovascular disease) to follow a medium-intensity physical exercise (eg walking with a fast pace) a minimum of 30 minutes, 5 days per week.
Are there other exercises that a person with a CKD can perform?
There are exercises that maintain the flexibility and others that have muscle strengthening as goal. Below are some examples of simple exercises. What is recommended, however, is for the patient to visit his physiotherapist and in collaboration with his nephrologist to create a personalized exercise plan.
Flexibility:
Circular shoulder movements

Neck stretches: turn right for 10 seconds and then turn left for 10 sec. NOT BACKWARDS!

Hand stretching

Hand pressure - Circular hand movements – Chest Press - Circular wrist movements
Quads stretch
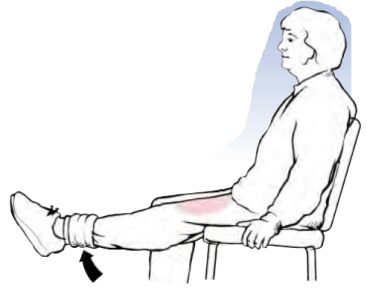
Calf stretch

Muscular Endurance Exercises
Quad Exercises

Quads Exercises

Upper limb exercises
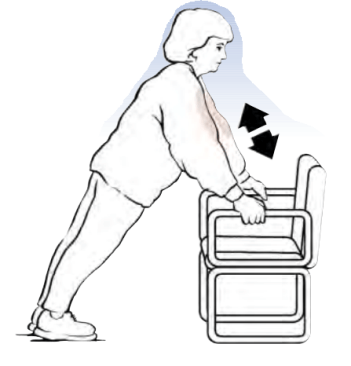
By the Scientific Director Aristides Paraskevopoulos
Bibliography
1: Hannan M, Bronas UG. Barriers to exercise for patients with renal disease: an integrative review. J Nephrol. 2017 Jul 8. doi: 10.1007/s40620-017-0420-z. [Epub ahead of print] Review. PubMed PMID: 28689231.
2: Bronas UG, Puzantian H, Hannan M. Cognitive Impairment in Chronic Kidney Disease: Vascular Milieu and the Potential Therapeutic Role of Exercise. Biomed Res Int. 2017; 2017:2726369. doi: 10.1155/2017/2726369. Epub 2017 Apr 19. Review. PubMed PMID: 28503567; PubMed Central PMCID: PMC5414492.
3: Morishita S, Tsubaki A, Shirai N. Physical function was related to mortality in patients with chronic kidney disease and dialysis. Hemodial Int. 2017 Apr 18. doi: 10.1111/hdi.12 564. [Epub ahead of print] Review. PubMed PMID: 28418625.
4: Zelle DM, Klaassen G, van Adrichem E, Bakker SJ, Corpeleijn E, Navis G. Physical inactivity: a risk factor and target for intervention in renal care. Nat Rev Nephrol. 2017 Mar;13(3):152-168. doi: 10.1038/nrneph.2016.187. Epub 2017 Jan 31. Review. PubMed PMID: 28138130.
5: Hirai K, Ookawara S, Morishita Y. Sarcopenia and Physical Inactivity in Patients with Chronic Kidney Disease. Nephrourol Mon. 2016 Apr 26;8(3):e37443.doi: 10.5812/numonthly.37443. eCollection 2016 May. Review. PubMed PMID:27570755; PubMed Central PMCID: PMC4983408.
6: Barcellos FC, Santos IS, Umpierre D, Bohlke M, Hallal PC. Effects of exercise in the whole spectrum of chronic kidney disease: a systematic review. Clin Kidney J. 2015 Dec;8(6):753-65. doi: 10.1093/ckj/sfv099. Epub 2015 Oct 20. Review. PubMed PMID: 26613036; PubMed Central PMCID: PMC4655802.
7. Physical Activity and Public Health in Older Adults: Recommendation from the American College of Sports Medicine and the American Heart Association Circulation 2007;116;1094-1105; originally published online Aug 1, 2007;
8. Staying Fit with Kidney Disease. National Kidney Foundation, https://www.kidney.org

